Stress fractures are a quite frequent condition among elite athletes but more difficult to suspect in amateur athletes. Sacrum and pelvis are infrequent locations for stress fractures and a high suspicion is required to consider them in a patient with gluteal pain.
Case reportWe present a 35-year-old male who consulted for gluteal pain that appeared 3 days prior whilst running a half-marathon. He was an amateur athlete, who used to run 5–6 h per week. He had run several marathons and half marathons in the past.
The gluteal pain started during the last 3 kms of the race, without any falling or limping.
The physical examination showed mild limping, pain while walking, increased pain when palpating the deep gluteal compartment and with hip internal rotation.
Musculoskeletal ultrasound was performed, showing a little amount of liquid around the proximal insertion of pyramidal muscle and cortical irregularity of the sacrum around the pyramidal insertion.
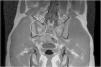
Suspecting a sacral stress fracture, an MRI was conducted, showing a transversal fracture of the sacroiliac joint (Fig. 1), bone edema and edema in the pyramidal muscle insertion.
Once diagnosed with a sacral stress fracture the patient was recommended to reduce impact activities for a month and progressively resume non-impact exercise/physical activity for another month.
The patient restarted running without pain and limitation, with the same frequency and intensity, 12 weeks after the injury.
DiscussionStress fractures are relatively frequent among runners (between 10 and 15 %.1), being the tibia and the metatarsal bone the most frequent locations.
Pelvic stress fractures constitute a 1 % of the total2 and the diagnosis is difficult to reach because of the limitations in the physical examination related to the affected body area. A high clinical suspicion is required in order to request the optimal diagnostic tests: MRI is the gold standard to diagnose stress fractures.2
There are scarce literature series on pelvic and sacral stress fractures, which limits the necessary evidence when talking about the therapeutical options.3 The latest Literature shows a higher number of these injuries amongst women, related with a decrease of the bone density.3 The presence of previous stress fractures is also a risk factor to have a sacral stress fracture. Vertical overload trough the lumbar lordosis seems to be the biomechanical factors related to these injuries, explaining why there is a greater incidence in impact sports such as long distance running or vertical jump. Also, an anterior pelvic tilt has been related to this vertical overload and stress sacral fracture.6
Pain tends to occur in the sacroiliac joint, triggered by palpation or impact physical activity. Some Patients can also report low back pain.3
Due to the characteristics of sacral stress fractures, the diagnosis can be delayed (an average of 6 weeks, with a maximum of 30 weeks according to a recent systematic review).5 The diagnosis is made by CT scan or MRI and the most frequent location is the iliac wing or the sacral body. Bilateral sacral stress fractures have been described.7
Differential diagnosis must include sacroilitis, vertebral fractures, disc pathology, trochanteric bursitis, spondylolisthesis, facets arthrosis, and lumbar or gluteal muscle injuries.
Regarding the treatment, all studies agree with an initial reduction of impact activities, with a progressive return to activity. In a 100-case series, the median return to activity was 7,4 weeks (5–40,5).4 In some cases, there was no resolution of the symptoms (persistent gluteal pain on physical activity after 2 years of follow up).4 Pain killers are frequently recommended in these patients and some studies have proposed the use of calcium and vitamin D, with controversial results. Calcium and vitamin D do have an effect in preventing stress fractures in case of deficiency, but do not reduce the progression of the injuries.8
In conclusion, sacral stress fractures are underdiagnosed, so they must be included in the differential diagnosis of lower back pain, gluteal pain and hip pain in impact sport athletes.